Subclavian Central Venous Catheter
INDICATIONS
- Central venous access for infusion of vasoactive drugs, TPN, high dose KCl, etc.
- Hemorrhagic disorder where large volumes blood/blood products needed
- Measurement of central venous pressure
- Need for frequent blood draws where peripheral access limited.
- Lack of peripheral venous access
CONTRAINDICATIONS
- Severe coagulopathy; INR > 1.5-1.6; platelets < 50 K (relative contraindication). The femoral or IJ site is preferred with a coagulopathy or anticoagulation due to the ability to compress the vein in the event of serious hemorrhage.
- Infected skin site
- In patients with higher risks for pneumothorax or inability to tolerate pneumothorax, the IJ or femoral sites may also be preferred.
RISKS
The risk of complications of central line placement varies with the experience of the operator and the conditions (emergency vs. elective) under which the line is placed. Nonetheless, some general statements can be made and used when obtaining consent from a patient.
Based on a 2000 meta-analysis of over 4000 central lines, the following figures may be useful in defining risks:
- Risk of Arterial Puncture
- Subclavian: 0.5%
- Internal Jugular: 3.0%
- Catheter malposition
- Subclavian: 9.3%
- Internal Jugular: 5.0%
- Hemo- or Pneumothorax
*
- Subclavian: 1.3%
- Internal Jugular: 1.5%
- Bloodstream Infection
- Internal Jugular: 8.6%
- Subclavian: 4.0%
- Vessel Occlusion/Thrombosis
- Internal Jugular: 0%
- Subclavian: 1.2%
*Note: Patients with COPD or ARDS were not included in study; previous estimates ranged from 1-5% incidence of pneumothorax. Whether subclavian lines have a higher rate of pneumothorax is questionable.
INDWELLING CENTRAL VENOUS CATHETER REMOVAL GUIDELINES
- No specific time interval for changing or removal. Catheter site and need should be reassessed daily. If site becomes infected, removal and if needed, replace at a different site.
- If line is to be removed because of suspicion of a catheter-related infection, and the skin site is not infected-looking, guide wire exchange with blood cultures through the line and culture of the tip should be performed
- Catheter removal may not be required with coagulase-negative Staph line infection without infected skin site, but most other catheter related infections require removal and antibiotics.
PREP & ANESTHESIA
- Place patient in reverse Trendelenberg position (head down)
- Move any ECG leads
- A towel between the shoulder blades is not necessary
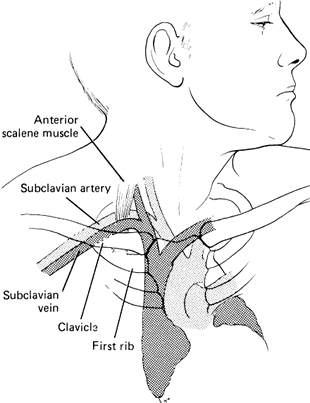
- Locate a spot 1-2cm below the clavicle where the proximal 1/3 and distal 2/3 of the clavicle meet.
- Cleanse a 15-20cm area with povidone-iodine solution;
- Drape the patient with the provided paper/plastic drape and turn the patient's head to the opposite side.
- Using the 25 ga (blue) needle, make a wheal under the skin at the desired spot, and anesthetize the subcutaneous tissue
- Using the 20 ga needle, anesthetize deeper, aiming towards the sternal notch.
- Make sure to anesthetize the inferior portion of the clavicle as this is the most sensitive area. Bump up against the lower third of the clavicle and serially numb it lower and lower. Always pull back before you inject to avoid intravascular injection of lidocaine.
TECHNIQUE
- Place the guide wire, dilator, catheter, and scalpel on the sterile drape for easy reach when needed.
- Estimate the length of catheter to be placed to end up with tip above right atrium
- Align the bevel of the needle with markings on the syringe to know which way it faces.
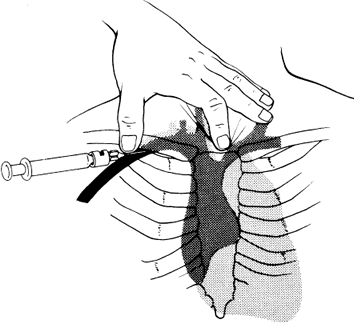
- Using the finder needle (largest needle in the kit) and a small syringe, enter the skin at a 30-45 degree angle, aiming towards the sternal notch, always pulling back gently on the syringe.
- When you see a flash and easy withdrawal of dark blood, this indicates entrance into the vein.
- If you bury the needle without blood, gradually withdraw; you may still get into the vein.
- Steady the needle and remove the syringe, holding a thumb over it to prevent air embolism.
- Rotating the needle so the bevel faces down may facilitate directing the guide wire into the inominate vein
- Insert j-tipped guide wire into needle; if resistance is felt do not force it.
- Watch monitor as guide wire is advanced. Ventricular ectopy indicates placement in RV, and guide wire should be pulled back a few cm. Generally 10-12 cm of guide wire should be placed beneath the skin to ensure entry into the vein.
- Holding guide wire, remove needle from skin.
- Make a small nick with the number 11 blade where wire enters skin to accommodate dilator.
- Advance dilator over guide wire with a twisting motion; there will be resistance.
- Remove dilator, holding guide wire
- Place catheter over guide wire; it should advance easily. Hold guide wire at skin entrance and feed it back through distal port of central line. When wire comes out, hold it at the end and finish advancing catheter.
- Remove guide wire and flush line.
- Suture catheter in place via flange with holes. If more than a cm or 2 of catheter is exposed due to length, either suture the catheter down or use the snap-on flange provided in the kit This will prevent migration of catheter further into vein.
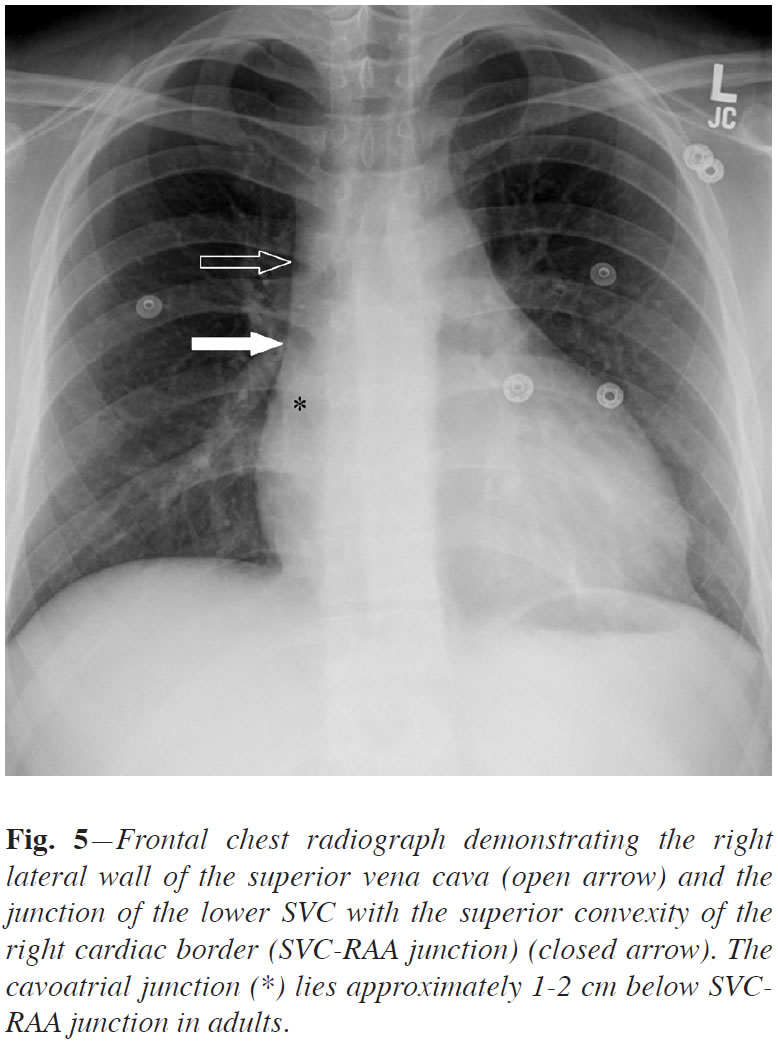
- Order a stat CXR to evaluate for line placement and complication. The tip of the catheter should be at the junction of the SVC and right atrium on chest xray. New data would suggest that this is 2cm below the superior right cardiac sillhouette which is made up by the right atrial appendage. (Verhey P.T., Gosselin M.V., Primack S.L., Blackburn P.L. and Kraemer A.C. (2008) The Right Mediastinal Border and Central Venous Anatomy of Frontal Chest Radiograph - Direct CT Correlation. Journal of the Association of Vascular Access. 13(1), p.32.) Advancement beyond this point can lead to arrythmia and unlikely myocardial perforation.