The IMBUS Program Background
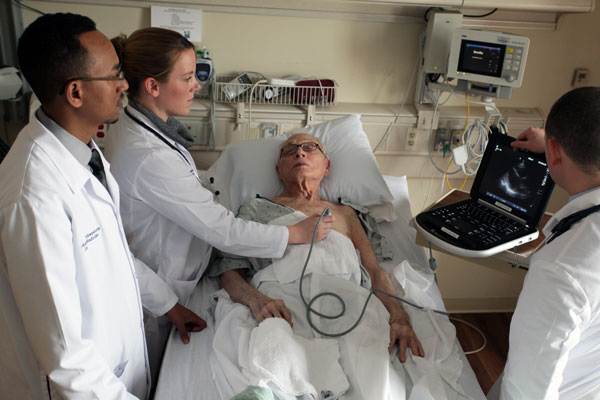
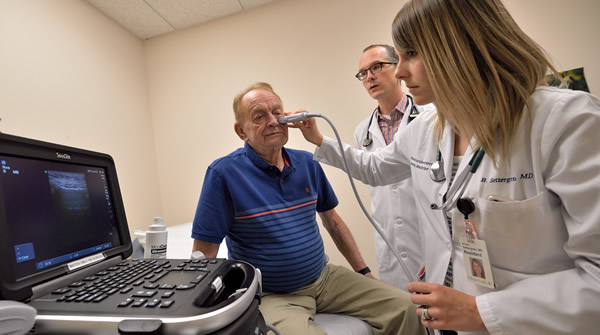
Our residency program has moved well beyond using bedside ultrasound for invasive procedures, which it has been doing extensively since 2006, and in 2010 we began a full 3-year curriculum integrating bedside portable ultrasound into the physical exam through a program we call IMBUS (Internal Medicine Bedside UltraSound).
We are among a growing, but still small group of Internal Medicine residency programs nationwide that have embarked on this mission that we feel is essential to the future careers of our graduating physicians and faculty. There is a global push for using ultrasound preferentially over other radiation-based imaging modalities when able. The goal of IMBUS is not to replace diagnostic radiology, formal cardiac echocardiography, or the important aspects of the classic physical exam, but rather to improve our bedside diagnostic accuracy and efficiency in areas where the classic physical exam and radiology-based imaging is insufficient. Additionally, bedside ultrasound provides immediate feedback to our classic physical exam elements, thus improving their accuracy for times when ultrasound is not available. Finally, it provides our internal medicine residents with a solid foundation for a career skillset that will one day be as widespread as that of the stethoscope.
Across the country, medical schools are integrating ultrasound training from day 1 of medical school. Over the next decade, this will become a standard across high-quality student, resident, fellow, and faculty training programs in the United States, as it already is in many parts of Europe. Since we started the IMBUS program in 2011, we have seen a rapid increase in the number of internal medicine residencies starting bedside ultrasound programs and routinely provide guidance/consultation for programs starting curricula.
Unfortunately there are many hurdles to the implementation of an internal medicine ultrasound program in a training environment. As a result, there are very few programs that have successfully implemented a full inpatient and outpatient program across both its faculty and residents. We have consulted with many programs across the country in an effort to help them implement a successful program at their institution and work through these hurdles.
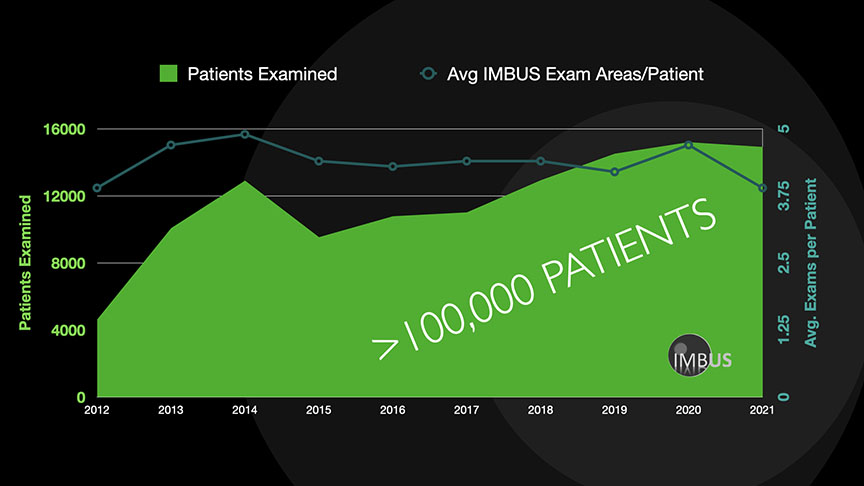
To date, the IMBUS program has trained 90 residents and 80 faculty (inpatient/outpatient). Those physicians have together performed over 70,000 focused bedside ultrasound exams (updated 6/2018).
The IMBUS Curriculum & Certification
The 3-year curriculum is one of the most robust and long-standing in the nation. The program consists of a rigorously overseen instructional and evaluative program of didactic and hands-on components concentrating on areas of our current physical exam that lack sensitivity and specificity amongst today's internal medicine physician and our patient population. Examples include: assessment of organomegaly, pulmonary processes such as pneumothorax, pleural effusion, pulmonary edema, and pneumonia, volume assessment and gross cardiac function, acute assessment of the critical patient, outpatient musculoskeletal and HEENT ultrasound, and several other areas of internal medicine that demand the highest accuracy and efficiency of diagnosis at the bedside.
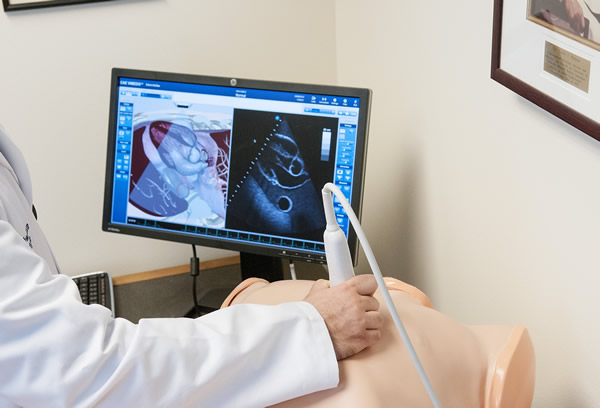
Training is multifaceted, however the core initial training for our incoming G1 residents is a one-week bootcamp early in the first year when they are removed from their clinical obligations to complete this 40-hour training course that the residency faculty teaches. Ongoing training at the bedside, advanced lectures, and our IMBUS case conference adds to the training throughout the year. Residents have a dedicated month of ultrasound during the Procedures & Ultrasound rotation where they work 1-on-1 with the ultrasound director and 2 other core hospitalist ultrasound/procedure staff.
Importantly, and uniquely, the use of ultrasound in our outpatient internal medicine clinics is just as robust as the inpatient environment. Our clinics have 4 ultrasound units in them and dedicated ultrasound exam rooms. During all 3 years of training residents receive dedicated outpatient ultrasound training in our clinics, and participate in an intensive G2 outpatient ultrasound curriculum 4 half-days a week during their outpatient rotation. There are many nuances of ultrasound that exist in the outpatient environment compared to what is seen inpatient, thus this is an imperative component of a well-rounded internal medicine point-of-care ultrasound training program.
Residents are certified in each ultrasound component with rigorous analysis of their individual testing characteristics prior to performing the exam component on their own and using it for medical decision making. All exams performed on the residency's 13 portable ultrasound machines are wirelessly transferred to the IMBUS our online PACS system and reviewed by the IMBUS program director with feedback given when necessary to the performing resident/faculty member. In 2013 through support from the hospital and the ANW Foundation, a portable ultrasound machine was put into place on every floor of the hospital and in all of our outpatient clinics making ultrasound readily accessible in any location.
Another Step Forward in 2017: machines in our pockets
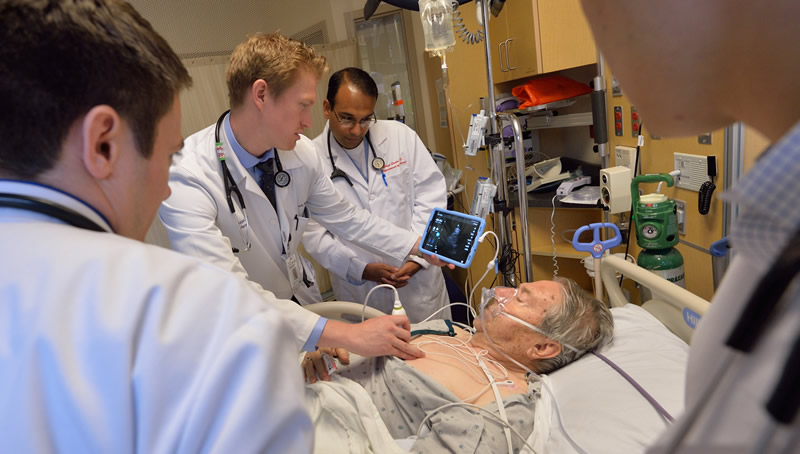
In 2017, the IMBUS program acknowledged the increase need for, and educational benefit of tablet-sized portable ultrasound machines residing in residents' pockets. The program added tablet ultrasounds to all of our inpatient resident ward teams and ICU teams. One of the major inhibitors of resident skill acquisition is number of repetitions. These repetitions are directly related to the proximity of a machine to your daily workflow. Even when machines are located on all of our hospital floors and clinics, an increase in use and learning is seen with the proximity of machines in your coat.
TrackUS: learner tracking & credentialing system
The faculty and residents record all of their ultrasound exams remotely on our smartphone application created for the individual tracking and credentialing of ultrasound learners within the IMBUS program. Details of this application presented at the World Congress on Ultrasound in Medical Education in 2014 can be seen here.
The 2014 conversion of the application to a fully customizable, web-based, and platform independent tool, "TrackUS," will allow use by other training programs in need of a comprehensive solution for gathering and analysis of point-of-care ultrasound user data. An in-depth overview video of the TrackUS application can be found HERE for programs and medical schools looking for a point-of-care ultrasound tracking system that can be customized to their program.
The IMBUS Faculty
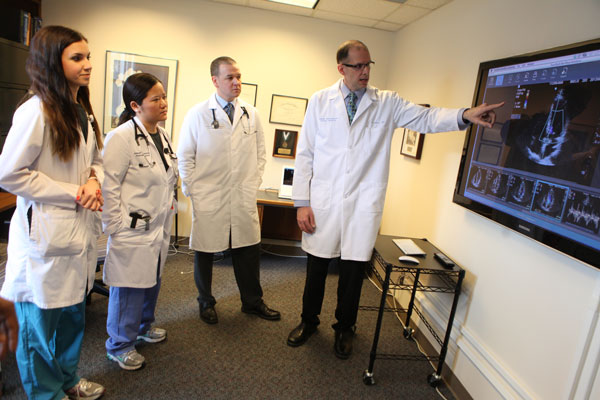
One of the most difficult hurdles we encounter when consulting with other programs implementing an ultrasound training program is how to get enough Internal Medicine faculty experts trained so that the residents are surrounded by teachers. We have taken the time over the last several years to ensure that our entire program leadership has been extensively trained in bedside ultrasound prior to training our residents. This ultrasound core faculty currently includes 12 Internal Medicine staff physicians including both inpatient and outpatient faculty. This ensures that you are learning this invaluable new skill in the correct environment.
Our faculty teach and present regularly national and international point-of-care ultrasound conferences and courses.
By the time you finish residency, portable ultrasound will be an expected skill in many areas of internal medicine, and will have replaced our stethoscope in many areas of our physical exam. We are dedicated to making sure that our graduating residents and faculty are trained to a standard in bedside ultrasonography far beyond that of most training programs that will allow them to be leaders in the field if they so wish.
IMBUS Research
There is extensive inpatient and outpatient research going on within the residency program around the use of point-of-care ultrasound for internal medicine. This research involves collaboration with multiple institutions across the country as well as with our local ultrasound partners at Abbott Northwestern such as the Minneapolis Heart Institute (Cardiology).
The IMBUS-PCI study is a 5-year, 16,000 patient study looking at the "big picture" outcomes of internal medicine use of ultrasound in the hospital setting. These outcomes include, cost of care, resource utilization (radiology studies, antibiotics, etc.), length of stay, ICU length of stay, patient satisfaction and disease understanding, etc. This study will hopefully quantify the anecdotal evidence we have over the last 5 years for the impact that we know the IMBUS program has.
There are many inpatient IMBUS studies in progress, however our outpatient clinics are also actively engaged in research focused on common outpatient internal medicine areas such as ultrasound for sinusitis, the integrated ultrasound physical exam for internists, point-of-care ultrasound and blood pressure management, etc.
See recent IMBUS scholarly publications HERE.
IMBUS in the media
Return to the Bedside Perspective Article - 2018
AIUM/ACP/SUSME Internal Medicine Residency POCUS Webinar - 2018
SonoSim Case Study
Apple/Filemaker Customer Success Story & Video
Beckers Hospital Review
Minnesota Medicine (page #28)
iBusiness (page #23)
Health Management Academy Case Study Volume 1
Health Management Academy Case Study Volume 2