The Inpatient Resident Service
There are six general ward and one ICU internal medicine resident teams comprised of a senior (G2 or G3) resident, a G1 resident, and 2 third-year medical students from the Univ. of MN. The ward teams manage a variety of general medicine and subspecialty patients, all under the supervision of a dedicated hospitalist or residency faculty physician. The ICU resident team works under the supervision of one of the Intensivist attendings.
Attending Teaching Rounds
All of the Residents' Service patients are the direct responsibility of full time faculty physicians. Subspecialty physicians are consultants for these patients. Faculty attending physicians give residents primary responsibility for patient care. All of a resident team's patients are with a single hospitalist faculty attending and a portion of the patients are geographically centralized.
Each resident team has separate daily teaching rounds with its teaching attending to provide optimal learning for the residents. Our system maintains an ideal balance between the need for resident responsibility and autonomy and the need for appropriate supervision and education by experienced, knowledgeable clinicians.
Attending Rounds Technology
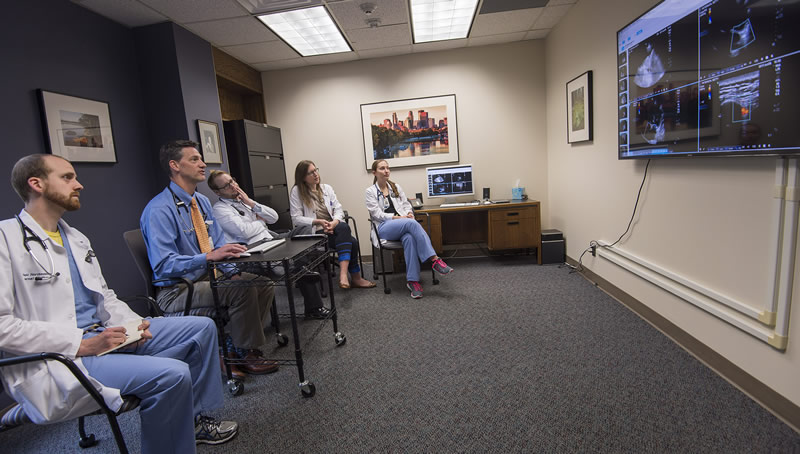
The online availability of the computerized medical record and the digital radiology (including our resident ultrasound image server) system on large screen displays in each of the attending rounds rooms make these daily teaching sessions in-depth, precise and interactive. In addition, it allows the attending to access any online resources to answer questions, or to access our audiovisual database of items such as physical exam findings, peripheral smears, ECGs, etc.
Unit and Team-Based Rounding
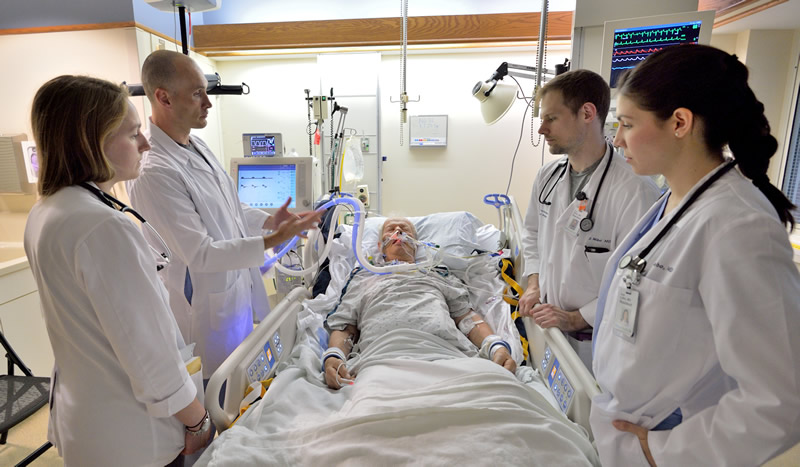
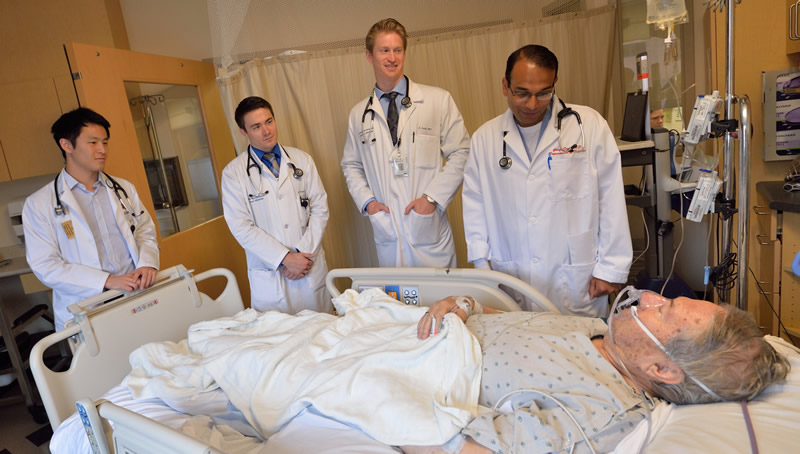
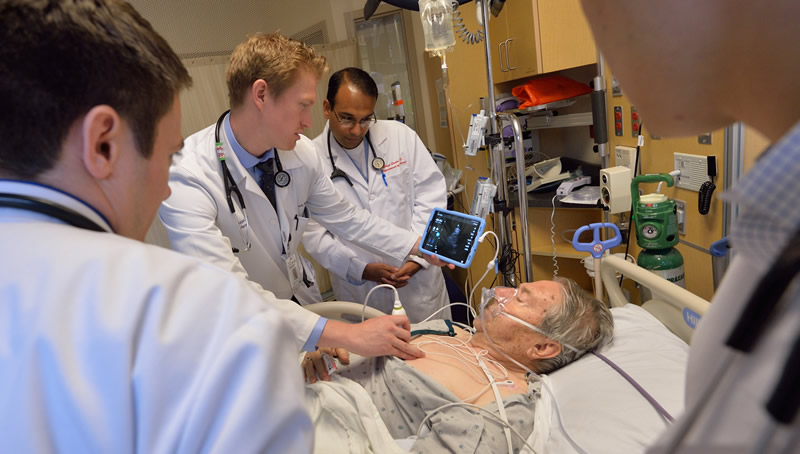
On ward rotations, residents participate in unit-based rounding with their teaching faculty. This allows residents to work closely with designated faculty physicians as a team in geographically focused areas in general medicine and a separate ICU team under the supervision of intensivists. This model has a number of important advantages that better meet the needs of patients in today’s hospital setting. It enhances communication among all caregivers, provides more efficient and coordinated care, and allows for multidisciplinary rounding. The system also facilitates more bedside teaching, strengthens faculty-resident feedback, and promotes the performance of mentored bedside ultrasound.
Residents also rotate through the core residency faculty inpatient service. On this service a resident team cares for a variety of patients with a faculty member who is rounding on the groups’ inpatients. Residents are thus able to take advantage of a service managed by skilled staff physicians who practice both in the clinic and in the hospital. This model enhances the resident experience in caring for patients in a system that promotes well-coordinated transition and post-hospitalization care.
This mix of inpatient experiences represents the current and future of hospital-based medicine, and ANW residents are able to benefit from a team-based structure that optimizes patient care, resident learning, and positions them well for practice.
Call, Admissions and Workload
Resident teams are on long call every sixth day/evening while on inpatient ward rotations. The long call team does not stay in the hospital overnight and leaves no later than 11pm. The G2/G3 on long call is also the leader of the in-house code/resuscitation team. There is no night call responsibility during non-ward rotations except for limited night float during the first year. All ward rotation residents have 1 day off per week during ward rotations and that day occurs on a weekend day. During long call, a ward team admits a maximum of 5 new patients. G1 and G2/G3 residents from each team are always on call and admitting together to provide optimum continuity of patient care and learning.
Besides one long call day in each five-day cycle, each team has one short call day. On a short call day, teams admit a maximum of two new patients who must be in the hospital by 3 p.m. A "trickle" admission/pickup process is in place to assure balanced team size and workload on all days except for long call and post-long call days. Our average 2-resident/2-medical student team size of patients is 9-10 and our maximum team size is 12 patients. Our average team sizes increase twice during the academic year to maximize effiency as residents improve during the 12-month academic year.
Night Float System
The night float system provides additional nighttime coverage for the patients on the Residents' Service overnight. An in-house G1 resident on the Night Float rotation provides cross coverage from 10pm to 8am. The long call team is not responsible for cross coverage, and is therefore able to focus on new patient evaluations and completion of their call day at a reasonable hour. The long call G2/G3 resident and moonlighters are both available to help the night float G1 when needed. Hospitalist faculty, intensivists, and cardiologists are in-house 24 hours a day when further assitance is needed.